The GP Patient – 5 Fast-fire Tips to Keep Communication Constant
Posted in Digital Healthcare Insights
The pandemic has shown us all just how critical digital lines of communication can prove.
In normal circumstances, multiple communication streams can build relations and improve patient engagement. But during an emergency, being able to drive a message home quickly can mean patient outcomes are protected, despite hell breaking loose.
1. Communicate at ALL times with patients and staff
Do so even when there is no news, because people feel connected. When the time comes that you really do need to communicate – like in the midst of a pandemic, people will be ready to listen.
2. Open as many lines of digital communication as possible
Like email, social, and text. While some patient groups won’t have smartphones nor own a computer, a growing number of older patients are now found on these mediums (one in five over 75’s now own a smartphone, while 35% are active on social media.
3. Get to grips with the official social media guidance from the GMC
But don’t be afraid to use social media. 74% of internet users engage on social platforms. 80% of those users are looking for health information, with nearly half searching for information about a specific doctor or health professional.
4. Embrace the power of text messages
Texts can be used for everything from ad hoc news to appointment reminders; the latter of which has reduced DNA rates by as much as 30%.
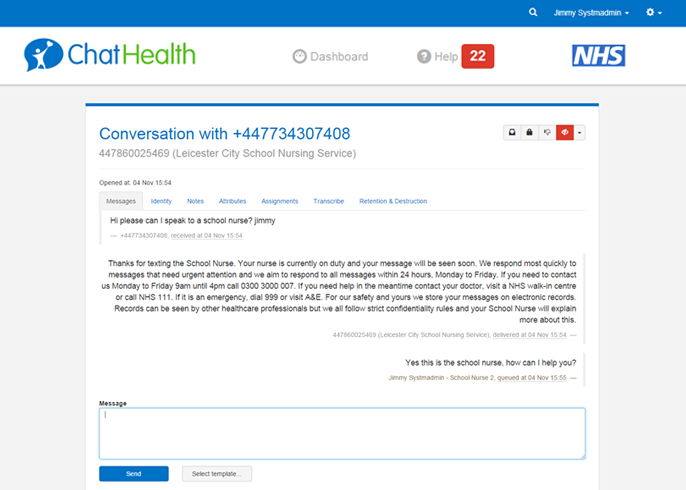
In some regions, the services that are accessible by text are more sophisticated. ChatHealth is one such example…
“A secure and confidential text messaging service for young people. It allows patients to easily and anonymously get in touch with a healthcare professional for advice and support”.
5. Make video and phone consultations the norm, not the rule
Remote consultations have played a critical role in maintaining care during the coronavirus crisis. Yet for some surgeries they were already in everyday use, including in one northern GP’s, which managed to reduce waiting times by 47% through telephone consultations.
With 22% of GPs reporting an average waiting time of more than three weeks, remote consultations should be routine, rather than exceptional.

Monthly Archives
- July 2023
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- October 2019
- September 2019
- August 2019
- July 2019

